What Is Dry Needling — And Is It Right for You?
The first thing most people say when they hear "dry needling": "Is that just acupuncture?"
The short answer is no — and the difference matters. Dry needling is a clinical technique rooted in Western medicine, performed by physical therapists, and specifically designed to address the muscular dysfunction that drives chronic pain, movement restrictions, and recurring injuries.
If you've been dealing with stubborn muscle tightness, a nagging injury that won't fully resolve, or pain that returns no matter how much you stretch — dry needling might be what's been missing from your treatment plan. Here's what you need to know.
What Is Dry Needling?
Dry needling is a treatment technique where a licensed physical therapist inserts a thin, solid monofilament needle into dysfunctional musculoskeletal tissue to reduce pain, restore movement, and address the root cause of injury. The needle carries no medication or injection — hence "dry."
The technique is rooted in Western medicine and musculoskeletal anatomy — not traditional Chinese medicine. It targets specific tissues based on clinical diagnosis: where you hurt, why you hurt, and what structure is driving the problem.
The result is often immediate — reduced tightness, improved range of motion, and decreased pain — though some patients experience mild soreness for 24–48 hours as the tissue responds to treatment, similar to the feeling after deep manual therapy.
The Full Scope: What Dry Needling Actually Targets
One of the most common misconceptions about dry needling is that it only treats muscle knots. While myofascial trigger point work is one component, a fully trained clinician uses needling across a much broader range of tissue types — each with a distinct mechanism and clinical purpose.
At Ascent Total Performance, our certified DPTs are trained in all of the following:
Trigger point (myofascial) dry needling — thin needle inserted directly into a taut band of muscle to elicit a local twitch response, release tension, and restore normal muscle firing. The classic entry point into dry needling, originally developed by Travell and Simons.
Peri-neural dry needling — needling around peripheral nerves to improve microcirculation, reduce neurogenic inflammation, and disrupt fibrosis in chronic nerve-related pain conditions such as carpal tunnel syndrome, thoracic outlet syndrome, and nerve entrapments.
Peri-vascular dry needling — needling around blood vessels to enhance local circulation, accelerate tissue healing, and reduce chronic inflammatory buildup in poorly vascularized structures.
Periosteal pecking — direct needling of bone surface (periosteum) used for chronic tendon insertions, bone stress pathology, and conditions where the bone-tendon interface is the primary pain generator. Particularly effective for chronic plantar fasciitis, lateral epicondylalgia, and tibial stress reactions.
Tendon and ligament needling — targeting the tendon body or ligamentous tissue to stimulate collagen remodeling and healing in chronic overuse injuries where conservative loading protocols have stalled.
Musculotendinous and teno-osseous junction needling — addressing the transition zones between muscle and tendon, and tendon and bone — regions that are frequently the true source of pain in conditions that are labeled as general "tendinitis."
Most patients who've had dry needling elsewhere have only experienced trigger point work. The full toolkit is significantly more powerful — and more precise.
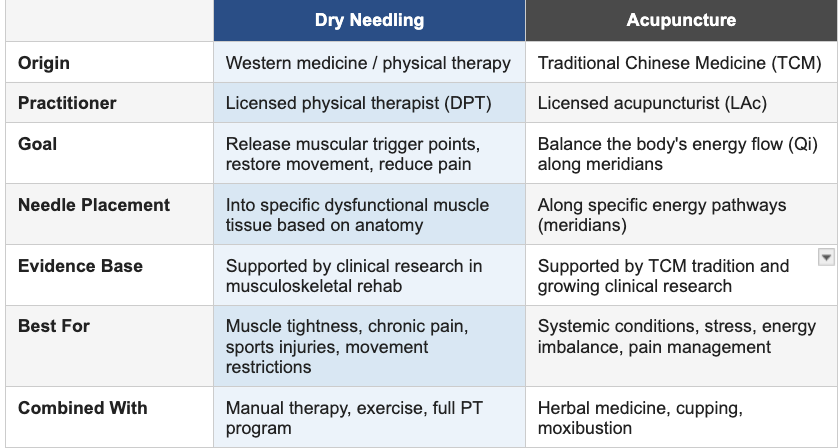
Dry Needling vs. Acupuncture: What's the Difference?
This is the most common question — and a fair one, since both involve needles. The answer comes down to origin, intent, and the training of the practitioner.
Both are valid, evidence-informed practices. But if you're coming in with a specific musculoskeletal issue — tight hip flexors affecting your squat, a rotator cuff that won't fully loosen up, chronic neck tension from sitting at a desk — dry needling performed within a physical therapy context is the targeted clinical approach.
What Conditions Does Dry Needling Treat?
Because ATP's clinicians are trained across the full spectrum of dry needling techniques — not just trigger point work — the range of conditions we can effectively treat is broader than what most patients encounter at other clinics. Common presentations include:
Neck pain and cervicothoracic stiffness — including desk workers, overhead athletes, and post-whiplash presentations
Low back pain — particularly when driven by paraspinal, quadratus lumborum, or hip muscle dysfunction
Shoulder impingement and rotator cuff dysfunction — including tendon and musculotendinous junction work
Lateral and medial epicondylalgia (tennis and golfer's elbow) — often requiring periosteal and teno-osseous needling at the insertion
Chronic plantar fasciitis — where periosteal pecking at the calcaneal insertion drives healing when loading alone hasn't worked
IT band syndrome and lateral knee pain in runners
Carpal tunnel syndrome and other nerve entrapments — addressed through peri-neural needling to reduce fibrosis and improve microcirculation around the affected nerve
Headaches and craniofacial tension — including suboccipital and temporomandibular (TMJ) presentations
Chronic tendinopathy — where collagen remodeling via tendon needling restarts a healing process that has stalled
Post-surgical scar tissue and muscle guarding — accelerating tissue recovery after procedures
Sciatica and lumbar radiculopathy — dry needling targets the muscular contributors to nerve compression and irritation, reducing the tension and inflammation that amplifies sciatic symptoms along the entire nerve pathway
TMJ dysfunction and jaw pain — needling the masseter, pterygoid, and temporalis muscles directly addresses the muscular hypertonicity driving jaw pain, clicking, headaches, and bite dysfunction in ways that splints and stretching alone often can't reach
Hip flexor, piriformis, and glute dysfunction — affecting gait, athletic performance, and low back loading
When the right technique is matched to the right tissue at the right stage of healing, dry needling can resolve presentations that have persisted for months or years — even when previous treatments have failed. The key is clinical precision, not just needling the spot that hurts.
Does Dry Needling Hurt?
This is the question everyone wants to ask but doesn't always. The honest answer: it depends on the muscle and how reactive the trigger point is.
The needle insertion itself is typically not painful — the needle is extremely thin, much finer than a hypodermic needle. What patients most commonly feel is the twitch response: a brief, deep cramping or aching sensation in the muscle as the trigger point releases. Most patients describe it as intense for a second or two, then immediately followed by a sense of relief or release.
First-time patients often say it was far less uncomfortable than they expected. The anticipation is usually worse than the reality.
Mild post-treatment soreness is normal and typically resolves within 24–48 hours. Staying hydrated and doing gentle movement after your session helps.
Most patients who were nervous before their first session ask to add dry needling to every session afterward.
What to Expect at Your Dry Needling Session at ATP
At Ascent Total Performance, dry needling is always performed by a Doctor of Physical Therapy — not an assistant, not an aide. Your entire session is one-on-one, which means your clinician is assessing and adjusting in real time based on your response.
Here's the general flow:
Movement and pain assessment — your DPT identifies which muscles are driving your symptoms and where the active trigger points are
Needle insertion — one to several needles are placed into target trigger points. You'll feel the twitch response in the muscle
Brief rest period — needles may remain in place for a few minutes to allow the muscle to fully release
Manual therapy and movement work — following dry needling, your DPT will typically follow up with hands-on work and movement patterns to reinforce the tissue changes
Home plan — you'll leave with specific guidance on movement, hydration, and any follow-up exercises
Sessions including dry needling typically run the full appointment time — you're not rushed through the technique and sent out the door. The needling is one component of a complete treatment session.
How Many Sessions Does It Take?
That depends on the chronicity and complexity of your condition. Many patients notice meaningful improvement after the first or second session. Longer-standing issues — chronic tightness that's been building for years, post-surgical tissue restrictions, or complex pain patterns — typically require more sessions to fully resolve.
Dry needling is most effective when it's integrated into a broader treatment plan. The needle resets the tissue. The manual therapy and exercise work change the pattern that created the trigger point in the first place. Without addressing the root cause, the trigger point often returns.
At ATP, the goal isn't to keep you coming back indefinitely — it's to resolve the issue at its source and give you the tools to stay ahead of it.
The Bottom Line
Dry needling is one of the most effective tools in a physical therapist's clinical toolkit for persistent muscular pain and movement dysfunction. When it's performed by a skilled DPT within a comprehensive treatment plan — not as a standalone quick fix — the results can be dramatic, even for patients who've tried everything else.
If you've been managing a chronic pain issue, a recurring injury, or muscle tightness that just won't respond to stretching and massage alone, dry needling may be worth exploring. The best first step is a thorough evaluation with one of our Doctors of Physical Therapy — so you know exactly what's driving your symptoms before any treatment begins.
📅 Curious if dry needling is right for your situation? Request an appointment at achieveatp.com and we'll evaluate what's driving your symptoms — and whether dry needling belongs in your plan.